Galatia, 40, does not know where she is, when she goes into labour. She has been walking for days through the Nuba Mountains in Sudan, carrying her pregnancy and leading seven of her youngest children along narrow bush paths, fleeing the war.
“I was so scared when I felt my baby come. I just saw someone on the path in front of me who took me into her hut when my daughter was coming,” Galatia remembers.

Miriam was born on the floor of a stranger’s hut. There was no clinic. No midwife. No clean water. When Galatia fled from conflict, she had hoped to reach a health facility in time, but she knew the risk of fleeing while eight months pregnant.
But there was no other choice for me. I thought I might find help on the way, but there were no one left.
By then, her home, Angolo village in Sudan’s Nuba Mountains, had already been bombed more than once. Bombs fall in the Nuba Mountains every day, tearing through houses and fields. There are almost no roads in the area. Villages are connected by narrow paths that vehicles cannot reach.
After birth, infection sets in. “My whole body ached, and I could hardly move out of bed,” Galatia says.
But there was no one there to give her the medicine or treatment she needed.
I stayed for seven days in the woman’s house who saved us. I was just so grateful that no bombs were falling at that time and that I could just breathe and pray that both of us, my daughter and I, survive this.
Seven days later, she left with a newborn in her arms.
I was living of the kindness of strangers. I did not have the right to overstay. The family was struggling themselves.
She tied her newborn to her chest and continued walking.
I was always thinking about my children and prayed that all will be good in the end. I hated that I could not keep them safe.

Impossible to survive at home
They avoided main roads. Armed attacks were common. They moved through bush paths instead. When it rained, they stopped to collect water from puddles.
I would not describe it as water. It was just something that was there and kept us alive, even though it made all of us sick. The water was full of sand and had a red colour.
She used an old oil jerrican to scoop it, pressing the opening to her children’s lips.
Behind her, her husband stayed with other men of the village to defend their home and give families time to escape. Months later, he was shot and killed. Neighbors brought the news.
They came here when they fled. Tears in their eyes. Carrying my husband’s clothes. I told the children that he was taken, and that they should keep up hope. I just could not tell them the truth. They learnt the truth after some time, when he still did not come to find us.
Today, Galatia sits in a small settlement just three kilometers from the Sudan–South Sudan border. Around her, other displaced families gather in a courtyard of self-built huts.

Her youngest children sit close, the now 2-year-old Miriam is unaware how close to death she and her mother came, on the road to safety. Galatia’s grandparents sort dried beans.
My grandparents arrived here three days ago. They did not want to leave Angolo initially, as they are too old for this hard walk. But the conflict has made it impossible to survive at home.

It is not only the violence. Crops cannot be planted. Food is scarce. Entire communities have left. Here, they plant the beans in the dry sand, which is not the good soil they are used to in the mountains. But it is enough to have at least one meal a day.
We cook the beans and mix them with water and have a very thin soup.
Galatia chose not to move deeper into South Sudan.
We are staying here, because we are too exhausted and scared to continue. I just cannot do this again with so many small children, and not my elderly grandparents.
The road to the next town, Yida – where there is a transit center, is too dangerous.
Many were already killed on that road.
She tried once, alone, hoping to find work. On the way, gunfire erupted. A young boy was killed in front of her on his motorbike. The driver of her truck was shot as well. She only survived because she ran away fast enough through the bushes.
This happens once or twice a month. I am too scared to take my family this way.
So, they stay.
A health facility as a lifeline
There is almost nothing in the settlement. No schools. No organised shelter. No regular food distribution. No jobs.
But there is one thing: a small health facility run by CARE.
The health facility is the reason we can survive here. I do not know what we would do without it. We cannot go back, we cannot continue. We are stuck here.

The facility helps refugees, returnees and the host community, when they are sick, too weak to continue, malnourished, injured or during pregnancies. A team of midwives, nurses, pharmacists, vaccinators, nutrition officers and lab technicians provide health services here directly at the border, just three kilometers from Sudan.
Galatia and her children also were helped here.
I had Malaria once and they helped me and gave me the medicine to get better again. Also, when my children were too malnourished, CARE helped us and they survived. Last week I had typhus and got treatment. I am the only one to provide for my children, if I die, they are all alone.
Across Sudan, the situation reflects her story at scale. Health systems have collapsed under the weight of conflict. Hospitals have been destroyed. Medical workers have fled or been killed.
An estimated 17.1 million women and girls now require humanitarian assistance. Among them are 1.1 million pregnant women. More than 4.3 million women and girls are displaced within Sudan, with millions more who have fled across borders.
Without access to care, women are giving birth at home under bombardment, on the road, under trees and in the bushes. The risks are immediate: hemorrhage, sepsis, obstructed labor. Stress, malnutrition, and displacement are also driving increases in preterm births.
Preventing death
Inside the CARE facility near the border, the conditions are basic. Next to the main structure stands a small grey tent: two by two meters.

Inside there is one delivery chair, a table with some medical equipment and a few buckets for water. The floor is covered with green plastic sheeting. A mosquito net hangs at the entrance for protection.
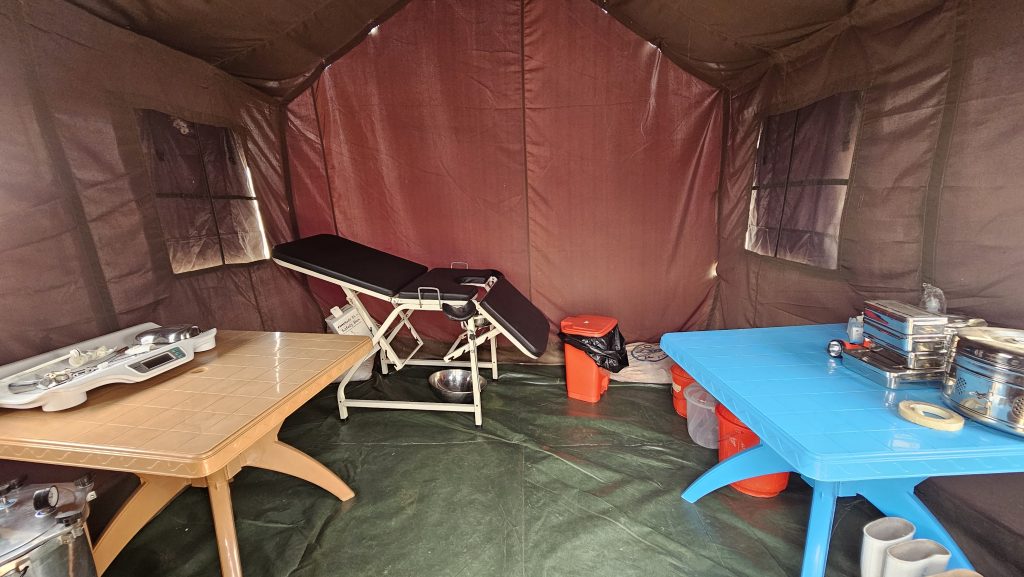
While temperatures outside reach 38°C. Inside, it is a lot hotter. “The sun is damaging the tent. It is nearly collapsing,” says Peter, CARE clinical officer.
We do not have the capacity for the number of deliveries we have here. Last week we had five women delivering their babies at the same time in this small space. Our midwives and nurses do the best they can with the limited resources, but it is very difficult for us and for the mothers.

The health facility treats around 30 to 40 patients every day. Mothers, pregnant women, sick, malnourished children, and those who are too weak to continue fleeing further come here every single day.
The health facility is the only point of access for humanitarian aid directly at the border in this area. No other aid organisations are here. So, this facility has grown to be the only lifeline for many people.
But time is limited as the project is only funded until June 2026 and Peter and his team are hoping every day that the project will be extended longer or that an alternative source of funding can be found in time.
If this program stops and the funding runs dry, then we will see many cases of mothers bleeding out after delivering their babies. With the abilities we have here, we have prevented death so far and I pray, that we can continue to support every mother who crosses the border fleeing this war searching for help.
This story has been written by Sarah Easter, CARE-Emergency Communications Officer
Want to contribute? Donate to CARE Australia today, or find more ways to give and support our humanitarians worldwide.